Introduction
For many expecting mothers, the joy and excitement of bringing a new life into the world are often accompanied by concerns about the birthing process. One specific area that generates a lot of anxiety and questions is the topic of perineal tears (also often called vaginal tears – these terms are often used interchangeably).
This article aims to address these concerns by providing in-depth information on the subject, including what perineal tears are, the degrees of tears, how they can be prevented, and tips for a speedy recovery. With this comprehensive from our expert midwife, we hope to alleviate your concerns and help you prepare better for birthing.
What is the Perineum?
The perineum is the area between the vagina and the anus. It is a part of the larger pelvic floor comprising a complex structure of muscles, ligaments, and tissues. This floor supports an array of internal organs such as the stomach, intestines, and kidneys, in addition to the reproductive organs like the uterus and ovaries. The entire pelvic floor has to expand for the baby to be born. The perineum plays a critical role during childbirth, stretching significantly, to allow for the baby’s passage.
Why does the Perineum tear?
During the birthing process, the perineum has the tough job of stretching to accommodate the baby’s passage through the vaginal canal. This stretching is so extreme that the perineal tissue may become as thin as paper. The stakes are high, particularly because the baby’s head – which is often the largest part of its body – puts substantial strain on the perineum as it moves through the birth canal. During this passage there is a chance that the perineum gives way and develops natural lacerations or tears.
According to statistics, about 33% of first-time mothers experience some degree of perineal tearing. If you’re preparing for childbirth, this statistic might sound alarming. But don’t worry; we hope that this article will give you all the information you need and help you prepare to reduce your chances of tearing.
What Are the Degrees of Natural Tears?
Understanding the different degrees of perineal tears can provide you with valuable insights into what to expect during childbirth and what care may be necessary afterward. Tears are classified based on the tissues that are affected, ranging from first-degree to fourth-degree tears.
First-Degree Tears: A first-degree tear affects only the superficial layer of the skin of the perineum and the vaginal floor. Unlike deeper tears, these do not involve the underlying muscles. While these are the most common types of tears, they are also the least severe. Most of the time, first-degree tears heal well on their own within a couple of weeks. However, some mothers request a repair if they are concerned about cosmetic changes in their vagina. At times, healthcare providers may recommend suturing if there’s notable bleeding, although this is generally rare.
Second-Degree Tears: Second-degree tears are deeper, extending beyond the skin to involve the muscle of the pelvic floor. These types of tears are also quite common and absolutely need medical attention for repair. Neglecting to do so can lead to functionality issues, including difficulties in bowel movements and sexual discomfort. Your care provider will usually use stitches to repair a second-degree tear, and recovery may take a few weeks.
Third and Fourth-Degree Tears: Third-degree tears extend further to involve the anal sphincter, while fourth-degree tears are the most severe, affecting the rectum as well. Both of these types of tears are comparatively rare but serious, requiring immediate medical intervention. Your care provider will likely use a specialized type of suture and may recommend additional treatments to ensure a complete recovery.
Most women experience first or second-degree tears during birth. However, with proper prenatal care, preparation, and in-the-moment techniques, the severity of these tears can often be minimized.
What are episiotomies?
What factors contribute to Perineal tearing?
Understanding what contributes to perineal tears can be the first step in preventing them. Therefore, before discussing prevention methods, it’s essential to understand the key factors that could increase your susceptibility to tears.
- Size of the Baby: The size of the baby’s head or body can impact the likelihood of perineal tears. A larger baby may put more pressure on the perineum, making it more likely to tear.
- Position of the Baby: The baby’s position during delivery can affect the risk of perineal tears. For example, if the baby is facing upward (occiput posterior position) or has an arm extended, it can increase the pressure on the perineum.
- Speed of Birth: A fast or uncontrolled delivery, often referred to as precipitous labor, can increase the risk of perineal tears because there’s less time for the perineum to gradually stretch.
- First-Time Births: Women giving birth for the first time are more susceptible to perineal tears because the perineal tissues haven’t undergone the stretching and expansion of prior births.
- Lack of Perineal Support: Insufficient perineal support from healthcare providers during delivery can contribute to tears. Healthcare providers can offer support, massage, and guidance to minimize tearing.
How to Prevent Tears?
While there’s no guaranteed way to completely prevent perineal tears, the following tips may help you reduce the risk:
- Nutrition: Lifelong nourishment plays a significant role in the health of the perineum. A diet rich in protein, fats, collagen, and Vitamin E, especially during pregnancy, can have a bearing on the condition of your perineum. A wholesome and balanced diet with a wide variety of healthy food can not only reduce your risk of tearing but also aid in faster and smoother recovery should a tear occur.
- Perineal Massage: While the jury is still out there about the efficacy of perineal massage, it’s advisable to perform perineal massage at least 3-4 times a week after 36 weeks. This technique may improve the elasticity of the perineum, reducing the chances of a tear.
- Using gravity and upright positions during birth: Imagine having a bowel movement lying on your back! We are sure you will agree that it is a very unnatural position. Similarly, lying on the back while pushing is not an optimal position for the mother and the baby. Women instinctively adopt upright positions like standing, kneeling on one leg, lunging, squatting, and on all fours. Following your body during birth can reduce your chances of tearing.
- Supporting the perineum during crowning: As the baby’s head fills up the vaginal opening (also called crowning), it works well if you were to reach down to support your tissues. If you are unable to or do not want to, then your care provider or spouse/birth partner can provide the support. This helps slow down the birth of the head and counterpressure on the perineum can sometimes help prevent tears.
- Lubrication: The vagina is a supple, lubricated part of the body. The discharge, and the amniotic fluid all provide extra lubrication during birth for the baby to slip out to be born. Sometimes, care providers may use fresh, virgin coconut oil or any other appropriate lubricant to stretch the tissues of the vagina and perineum.
- Breathing your baby out: the contractions during the second stage of labor are quite powerful and invoke a spontaneous urge to push in the mother. When the baby is crowning, instead of using a lot of force to birth the baby, you can use slow pushes, grunts, or deep breaths to ease the head out of your vagina. This is many times referred to as breathing your baby out.
How to Perform a Perineal Massage
Understanding the steps to perform a perineal massage can be a game-changer for mothers-to-be. Below, we’ve outlined an easy-to-follow guide that you can use or share with your partner.
Preparing for the Massage
- Clean Hands: Whether you or your partner are performing the massage, it’s crucial to start with clean hands. Wash your hands thoroughly with soap and water to ensure optimal hygiene.
- Mirror: If you’re performing the massage on yourself, a mirror can be incredibly helpful, at least initially, to guide you.
- Oil: Keep some massage oil like coconut oil or vitamin E oil handy. These natural oils are excellent for improving skin elasticity and will help reduce friction during the massage.
Position
- Semi-Sitting Position: If your partner is doing the massage, lie back in a semi-sitting position with cushions for support.
- One Foot on a Chair: If you’re doing the massage, stand with one foot elevated on a chair. This position provides better reach and comfort.
Step-by-Step Guide
- Application of Oil: Apply a generous amount of coconut or vitamin E oil to your thumb if you’re massaging yourself, or to your partner’s index finger if they are assisting.
- Initial Insertion: Insert the thumb (or partner’s index finger) into the vagina, up to about the second knuckle.
- Pelvic Floor Muscles: Do a few Kegel exercises to feel your pelvic floor muscles tense up and then relax. Understanding your pelvic floor muscles is crucial for effective massage.
- Massage Movement: Relax your pelvic floor. Curl thumb or index finger (in case of partner) and gently pull it outward and downward towards the anus. After reaching the outer limit, sweep it back in a rhythmic U-shaped motion inside the vagina.
- Breathing and Relaxation: As you or your partner perform the massage, concentrate on deep breathing. This helps to relax the pelvic floor muscles and prepares them for stretching during childbirth.
- Pressure: Apply pressure only to the extent you are comfortable with. The sensation should be a slight stinging or burning, similar to what you’ll experience as your baby’s head is born. As you get accustomed to the massage, slowly increase the pressure.
- Duration: Aim to continue the massage for about 3 minutes each time and try to incorporate it into your routine at least 3-4 times a week starting from the 36th week of pregnancy.
The massage should not be painful. If in doubt, please contact us at Veira Life and we can help you troubleshoot.
Note for Readers:
The infographic attached provides a visual summary of these steps for easier understanding and quick reference.
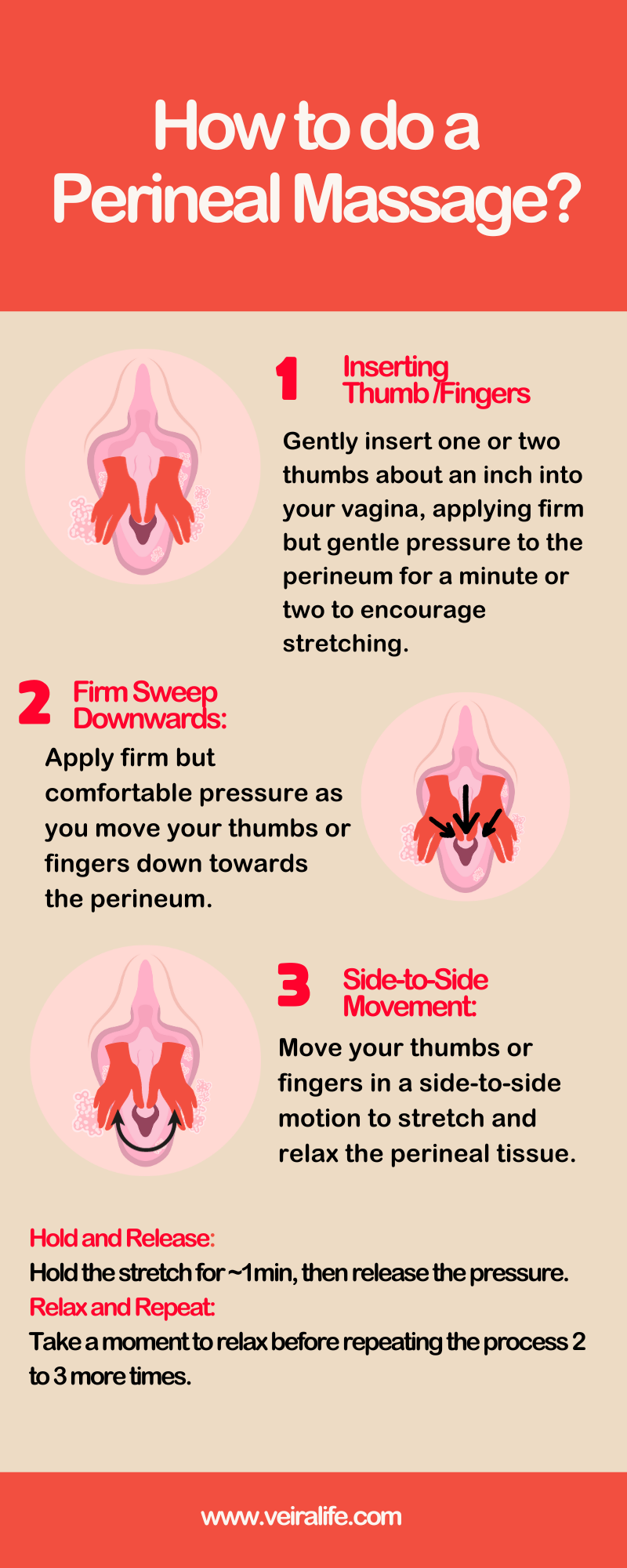
What to Expect During Repair in Case You Have a Tear?
If you do experience a perineal tear, don’t worry; most women don’t feel it happening. Immediately after birth, your care provider will assess the tear’s severity. For second-degree tears or episiotomies, suturing is usually required. During this time, focus on bonding with your newborn—whether that’s through breastfeeding or simply holding them. Your partner can also be there to support you, making this a family moment.
You’ll receive a local anesthetic to numb the area, so you’ll only feel a slight tugging sensation but no pain. In rarer cases of more severe third or fourth-degree tears, a stronger anesthetic known as a pudendal block may be administered for the repair process.
Healing from Perineal Repair
While natural tears often heal quickly without intervention, taking some precautionary measures can expedite the recovery process. Here are some essential tips for effective healing:
- Tear Grades and Healing Time: First-degree tears usually heal on their own within 2-3 weeks, while episiotomies may require 4-6 weeks.
- Cold Pads: Use cold pads (also known as padsicles) to help bring down inflammation. Padsicles can be prepared during pregnancy using the following simple steps:
- Take at least 20 sanitary or maternity pads
With clean hands, open them and pour 2-4 tbs of filtered water - Optionally you can add a few drops of good quality lavender essential oil and 1 tbsp of witch hazel.
- Fold up the pads and put them in a zip-lock bag, seal the bag, and put it in the freezer
- Use them often after birth, we promise you, they feel heavenly!
- Rest and Positioning: Aim for 2 weeks of bed rest and keep your feet together as much as possible to avoid strain on the perineum. Refrain from sitting cross-legged.
- Infection Signs: Be vigilant for symptoms like foul-smelling discharge, fever, or inflammation, which could indicate an infection.
- Stool Softeners: Utilize stool softeners to prevent straining during bowel movements, further aiding the healing process.
Conclusion
How Can Veira Life Guide You Through Preventing Perineal Tears?
Entering parenthood is a journey filled with joy, anticipation, and challenges. At Veira Life, we’re committed to helping you experience the best possible start. Our comprehensive prenatal classes offer you detailed guidelines and resources, including expert tips on preventing perineal tears and ensuring a smoother recovery if they occur.
Every member that joins is assigned a dedicated Veira Coach—certified professionals in childbirth education, lactation counseling, and more—to address your questions and provide personalized support. Your Veira Coach can help you navigate the complexities of perineal care, ensuring that you’re not just healing but also thriving on your journey into motherhood.
Are you looking to have an informed, empowered childbirth experience? Register with Veira Life today to give yourself the best start on your journey to parenthood.
Our Guide to Prevent Perineal Tears by Coach Chetna – Watch Below!
FAQs
Perineal tears in childbirth result from stretching due to the baby’s passage, baby’s size, positioning, and speed of delivery. First-time births and inadequate support can also increase the risk. In some cases, episiotomies are performed to prevent extensive tearing. Postpartum care is vital for healing and pain management. Consult a healthcare provider for personalized treatment.
The healing time for a vaginal tear varies based on the tear’s severity. First-degree tears may heal in a few weeks, while more severe tears like third or fourth-degree tears can take several weeks to months. Proper care and medical attention are essential for healing and reducing complications.
Natural plant-based oils like coconut oil, olive oil or sweet almond oil, can be used to perform perineal massage during pregnancy. Perineal massage may help increase the flexibility of the perineal tissues and reduce the risk of tearing during childbirth. Effectiveness can vary. Consult with your healthcare provider first to ensure it is safe and appropriate for your specific situation.
Perineal tears can often heal naturally, especially if they are minor. In such cases, stitches may not be required. Using an ice pack can alleviate pain and reduce swelling in the perineal area. However, the comfort level during recovery varies based on the severity and length of the tear.
Absolutely, walking can be beneficial for perineal tears, especially if you’ve experienced a third- or fourth-degree tear. Balance is key: mix periods of rest with gentle walks. However, avoid lifting anything heavier than your baby for the initial 6 weeks to aid in your recovery.

Author Bio
Chetana is a skilled and passionate Childbirth Educator trained in the Lamaze philosophy of childbirth preparation. She is also a Lactation Educator-Counselor and practicing midwife. She has developed a holistic childbirth preparation course which she has delivered to hundreds of families and has founded a highly rated natural birth center in Bangalore, India. She has over 11 years of experience supporting families through their journey and transition into parenthood.







